Could artificial blood save us from a global blood shortage crisis?
02 Apr, 20264+ minutes
At the start of 2026, the American Red Cross declared a severe blood shortage due to a 35% drop in blood supplies. Across the country, hospital requests are exceeding what’s currently available, meaning more people are dying from preventable deaths (the leading cause of death in Americans aged under 45).
This is a crisis that extends far beyond the U.S. The majority of the world’s people live in ‘blood deserts’, areas where the clinical need for blood cannot be met in at least 75% of cases. In low-income countries, more than half of the global population is living without access to basic, life-preserving resources.
The resulting effect is devastating. Blood is crucial for keeping people alive and is often considered one of the most critical medical resources. It’s used to treat victims in accidents, mothers enduring difficult childbirths, cancer patients – and is needed in bulk following military conflicts or bombardments.
Without blood, people die needlessly. Current predictions state that 2 million deaths are caused each year from traumatic hemorrhage (dying from bleeding out), and unless we find some sort of solution, this number will only rise given the aging population.
But not all hope is lost. Below we've highlighted several possible ways of tackling the blood shortage crisis as well as recent developments in the ‘holy grail’ of trauma medicine: a lab-made blood alternative.

The blood shortage crisis
The blood shortage crisis refers to the declining rates of accessibility to safe blood. With more than half of the world’s countries lacking reliable blood supplies, it’s not surprising that hemorrhage is the leading cause of death among trauma victims.
Blood availability starts with blood donors. Once collected, blood is tested for its type (A, B, AB, or O) and for potential diseases. It must then be stored in cold conditions and kept for no more than 42 days – as the blood will perish.
Getting blood from a donor to a patient isn’t a straightforward process. First comes the issue of transportation: keeping blood in the right conditions and equally distributing it to local hospitals and clinics.
Then, before a transfusion can safely take place, patients must have their own blood crossmatched with the donor’s blood to prevent adverse reactions (such as the body’s immune system destroying the foreign blood cells).
Blood transfusions require many steps – but that’s not the reason we are witnessing a global crisis.
Other factors are making blood availability even lower across the world, including:
- Poorer population health
- Higher rates of anemia and infection
- Less people actively donating blood
- Higher patient demand
- An ageing population
As older adults begin to make up a larger proportion of the population and younger donors decrease in numbers, the situation will become even more critical.

Short-term solutions
So, how can we make a difference to people’s lives when we are faced with a blood shortage crisis?
According to an article by Harvard Medical School, several short-term solutions have been proposed by the Blood D.E.S.E.R.T Coalition (which stands for Delivery via Emergency Strategies for Emergency Remote Transfusion). These include:
Civilian walking blood banks: Creating stations where civilian volunteers can give blood at short notice, so rural areas don’t have to solely rely on central storage.
Intraoperative auto-transfusion: A process that collects, filters and reinfuses a patient’s own blood, reducing the need for additional blood transfusions.
Drone-based delivery: A solution that would be very costly to implement safely –this idea involves the use of drones for transporting blood to remote locations.
While these solutions can’t replace a safe supply of banked, lab-tested blood, they have potential to save lives when there’s no other option.
Could we create a blood substitute?
There is another angle we can take regarding this crisis. If we are running out of traditional blood donations, why don’t we create a lab-based alternative?
In short, despite 150+ years of research into blood substitute products, we are still some ways from creating one. While the concept sounds straight forward, in reality it is immensely challenging to develop a man-made substance that successfully mimics the complexities of human blood. It’s sometimes referred to as the ‘holy grail’ of trauma medicine – a feat that has long felt out of reach.
This quest has seen many failures. There is, however, one exciting product (which received a $46 million investment from the United States military) that could be the answer we’ve all been waiting for.
ErythroMer, developed by biotechnology company KaloCyte, is a shelf-stable, field-deployable blood alternative that can be used in the absence of traditional, human blood. Using nanotechnology, the product is designed to mimic the function of red blood cells by carrying oxygen from the lungs to major organs and tissues – keeping patients alive in critical settings, often away from the hospital.
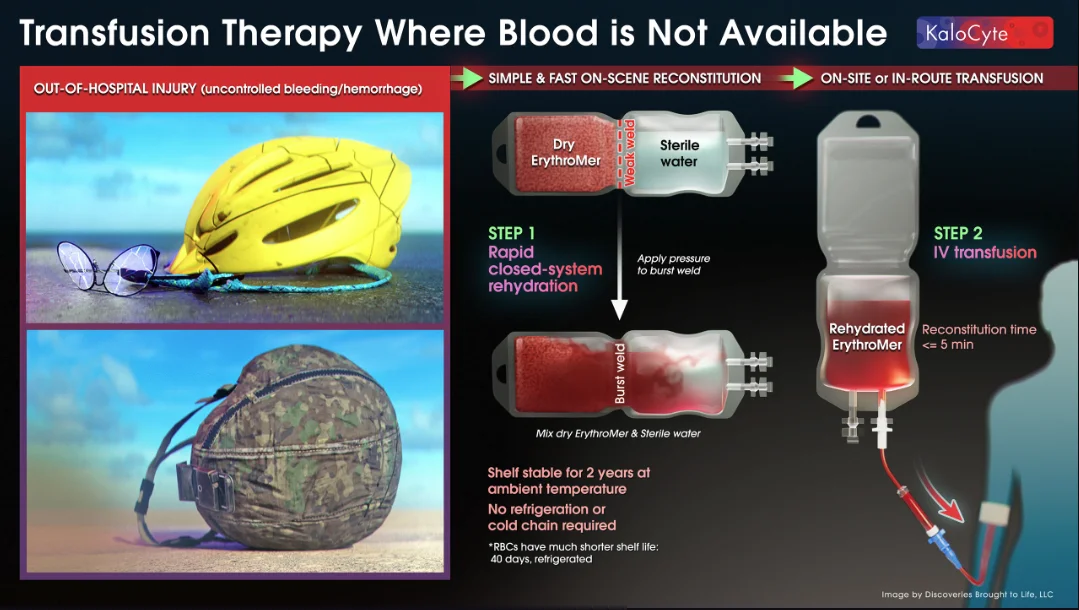
Unlike traditional blood which has a shelf life of 42 days, ErythroMer is freeze-dried and can be kept at ambient temperatures for up to two years. It also works universally on patients, which solves the problem of type sensitivity and its associated immune risk complications.
The company is currently at a pre-clinical stage but plans to progress towards first-in-human trials within a couple of years. If successfully brought to the market, their product will become a lifeline for when blood supplies are low, potentially saving millions. KaloCyte are certainly one to watch!
Efforts are also being made to synthesize lab-grown blood by creating human red blood cells in vitro. In recent years there were two noteworthy trials: researchers in Japan transfused a 55-year-old woman with lab-grown platelets and in the UK, a phase I trial involving cultured red blood cells in still ongoing.
While testing in humans is a huge step forward, we are still several years away from making this a standard practice. It’s also important to consider that lab-grown blood carries a significant cost which could slow down our progression towards larger, more widespread clinical trials.
Nevertheless, we are seeing tremendous progress – and the creation of artificial blood, whether it's an alternative like ErythroMer or a lab-grown kind, could provide a suitable, safe alternative as blood supplies continue to drop.